In the present world, we are all very focused on the various issues that could potentially improve our health. There are one million different diets and recommendations on how we could become healthier and slimmer. Caloric restriction is certainly a way to reduce body weight and fight overweight. Overall, a healthy diet is not necessarily vegetarian, vegan, low fat or low carb. Also eating regularly is probably healthier than (intermittent) fasting. But which diet is better than the other? What should we eat and when? Is there a universal recommendation that fits everyone? Probably not. Nevertheless, we can try to integrate personal preferences, feasible procedures in the kitchen and some inherited knowledge from our grandparents and maybe research findings from scientists.
The health of our organs is strongly influenced by what we eat. We are mostly aware of things that are not good for our body as for example sweets, soft drinks or fried stuff. And yes, there is evidence that high proportions of sugar and fat promote insensitivity to insulin, fatty liver, digestive problems and obesity. All these states are also only the starting point of developing diseases, which may become more prominent, compromising normal body functions and eventually leading to severe organ dysfunction. For example, clinical states of the liver are fatty liver (NAFLD), steatohepatitis (NASH), liver cirrhosis and finally hepatic cancer (reviewed in Anstee et al. Nat Rev Gastroenterol Hepatol. 2019)
In our group we are very much interested in the interactions of different players that contribute to health and well-being, but when misguided also drive development of metabolism-associated diseases. The composition of foods, the style the dishes are prepared, and the way we actually eat are one player and we refer to this as the diet.
In recent years many scientists worked on the question what is the gut microbiome, which bacteria compose the microbiome, how does the composition of the microbiome affect gut and liver function and how is that connected to metabolic diseases like type 2 diabetes and liver diseases. Another player, which became apparent in recent years, is the immune system, that is activated by specific diet- and microbiome-derived compounds and the term metaflammation was coined. This also drives the development of unhealthy body states and organ disease (reviewed in Christ et al. Immunity. 2019).
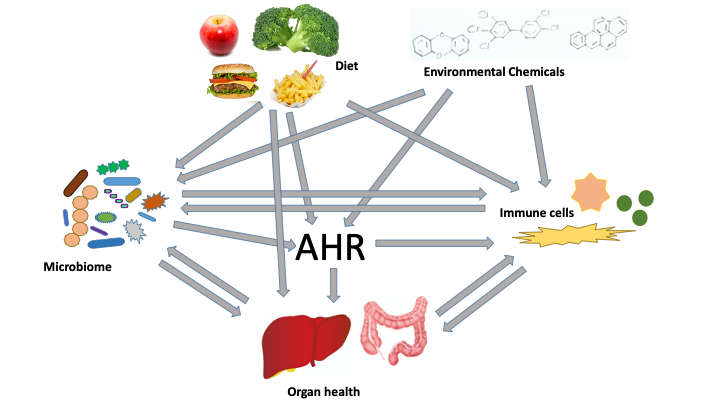
As shown in the figure, there is a complex interaction of the diet, the composition of the microbiome, the activation state of the immune system, environmentally derived chemicals, and all compounds derived from these players.
In the center of our research is the environmental sensor aryl hydrocarbon-receptor (AhR). It is a ligand-activated transcription factor, expressed in many cells of the body, including barrier organs and immune cells. Normal function of the liver and the gut is dependent on functioning AhR. In addition, AhR is required for development and normal performance of many immune cells (e.g. ILC3). The AhR serves as a sensor for signals in form of chemical compounds that may derive from the diet, the microbiome, environmental chemicals, and also metabolism in the body. It integrates all these signals to promote normal physiology and health through the actions of immune cells and through specific organ functions, as for example regulation of detoxifying enzymes in the liver. An interesting fact is that AhR may bind to a vast array of very different ligands from various sources and that these different ligands may induce different target genes. The AhR has the power to interfere with other signaling pathways, so that parallel stimulation with AhR ligands may lead to a somewhat different outcome of a signalling event.
However, many toxic substances are also bound by the AhR, for example Benzo(a)pyrene, which is present in cigarette smoke or 3-methylcholanthrene, known for its cancerogenic potential and also many drugs bind to AhR. In the liver, AhR induces oxygenase enzymes (e.g. Cyp enzymes); this is a very important process to eliminate harmful substances from the body (reviewed in Rothhammer & Quintana Nat Rev Immunol. 2019).
On the other hand, many substances derived from the microbiome and from the diet have beneficial effects on body health. To name two of them, indole-3-carbinol, present in broccoli (and other members of the cabbage-family Brassicaceae) and quercetin, an aromatic hydrocarbon found e.g. in apples and onions. These substances have been shown to improve organ health, especially intestinal and hepatic functions.
The interesting part for everyone who is eager to improve health and well-being is that natural ligands from the diet seem to have an organ-protective effect even under conditions of caloric overload. What is called a “Western Diet” (high amounts of sugar, simple carbohydrates, saturated fatty acids and salt) induces a metabolic syndrome, which describes obesity, hepatosteatosis, type 2 diabetes and related diseases. All this can be ameliorated by the consumption of natural AhR ligands.
The diet also shapes the composition of the microbiome: a healthy diet, containing AhR ligands, fosters a diverse and health-promoting microbiome, whereas “bad” foods, often devoid of AhR ligands may lead to outgrowth of a few commensals, which in turn may have detrimental effects on organ heath and immune cell functions. On the organismal scale, this has effects on how efficiently infections can be cleared and also on the probability to get cancer.
Having in mind the complex interactions of lifestyle, diet, the microbiome and the immune system that researchers discovered in recent years, we now have scientific evidence for what our parents always insisted on: We should really eat our Broccoli.

Author: Fabian Gondorf
